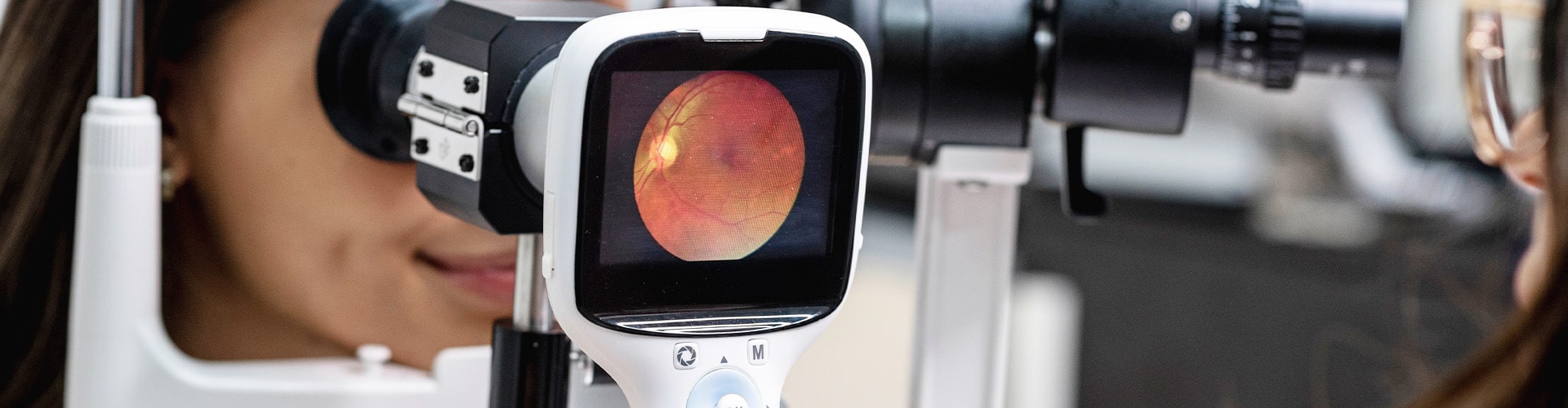
What is the Retina?
The retina is a very thin, but complex tissue that lines the back of the eye. It is composed of millions of cells, including photoreceptor cells that sense light and send images to the brain.
There are many conditions that can impair the retina’s ability to receive and transmit images. The most common retinal diseases are diabetic retinopathy, age-related macular degeneration and retinal detachments. These conditions are very serious, and if not treated, can lead to loss of vision.
Many retinal diseases can be treated with various forms of laser. These powerful light beams help destroy abnormal blood vessels in the retina or act to seal off retinal tears. Laser therapy is usually done in our office with anesthetic eye drops to ease any discomfort.
Learn about common retina conditions and how to protect your eye health with Griffey Eye Care & Laser Center.
Retina Conditions
Comprehensive eye exams help monitor retina structure and function changes to prevent retina problems. Take a closer look at a few common retina problems.
Diabetic Retinopathy
People with diabetes mellitus have difficulty using and storing sugar properly. High blood-sugar levels can damage blood vessels in the retina. Damage to these blood vessels is referred to as diabetic retinopathy.
A medical eye examination is the only way to detect changes inside your eye. An ophthalmologist can often diagnose and treat serious retinopathy before you are aware of any vision problems.
There are two types of diabetic retinopathy: nonproliferative diabetic retinopathy (NPDR) and proliferative diabetic retinopathy (PDR).
NPDR is an early stage of diabetic retinopathy where tiny blood vessels within the retina leak blood or fluid. Many people with diabetes have mild NPDR, which usually does not impinge on their vision. When vision is affected, it is the result of swelling or thickening of a small area in the center of the retina that allows us to see fine details clearly. This swelling is caused by fluid leaking from the blood vessels in the retina and is the most common cause of central vision loss in diabetics.
PDS is present when new abnormal blood vessels begin to grow on the surface of the retina or optic nerve. A widespread closure of retinal blood vessels causes the retina to respond and grow new blood vessels in an attempt to supply blood to the areas where the original blood vessels closed. Unfortunately, the new blood vessels do not supply the retina with adequate blood flow. These new vessels are often accompanied by scar tissue that may cause wrinkling or detachment of the retina, therefore causing visual distortion or loss. PDR may cause more severe vision loss than NPDR because it can affect both central and peripheral vision.
The best treatment is to prevent the development of retinopathy through strict control of your blood sugar. This will significantly reduce the long-term risk of vision loss from diabetic retinopathy. Early detection of diabetic retinopathy is key to protect against vision loss.
Laser surgery is often recommended for people with severe diabetic retinopathy. Multiple laser treatments over time are sometimes necessary although laser surgery does not cure diabetic retinopathy and does not always present further loss of vision.
Diabetics should schedule an exam at least once a year. Your ophthalmologist may require more frequent examinations if diabetic retinopathy is diagnosed.
Age-Related Macular Degeneration
Age-Related Macular Degeneration (ARMD) is a disease that affects the macula, the small area in the center of the retina that allows fine details in your central vision to be seen clearly. This slow progressing condition tends to develop as you get older, hence the term “age-related”.
There are two forms of macular degeneration: “dry” macular degeneration and “wet” macular degeneration. Dry macular degeneration is more common and is caused by aging and thinning of the cells in the macula. Vision loss is slow and gradual. Wet macular degeneration occurs in only 10% of patients and causes much more rapid vision loss. There is no cure for ARMD, however there are some treatment options for wet macular degeneration. Untreated wet macular degeneration can lead to scarring of the macular area and permanent vision loss. If you notice a change in your vision, i.e. telephone poles do not look straight or there is a section missing, please give our office a call at 757-410-9500 immediately to schedule an appointment.
Retinal Detachments
A retinal detachment occurs when the retina peels away from its underlying layer of support tissue. Oftentimes, a retinal detachment can be stopped by laser treatment. Some symptoms of a retinal detachment are:
- Flashes of light
- Sudden change or increase in the number of floaters
- A dense shadow that starts in the peripheral vision and slowly progresses toward the central vision
How are Retinal Diseases Diagnosed?
A dilated retinal examination is the only way to properly diagnose retinal problems. Serious diseases can often be treated before the patient begins to experience vision problems. In some cases, additional testing is required.
One test is the Optical Coherence Tomography (OCT), which is a new technology. This device bounces light rays off the retina and the reflections are transmitted to a computer, giving us a detailed 3D cross-section of your retina, showing:
- The impression of a dark curtain over your vision
- Straight lines appear curved
- Central vision loss
If you experience any of these symptoms or any sudden changes in your vision in general, you need to be seen as soon as possible. A retinal detachment is an emergency and requires immediate attention.
Monitor Your Retina Health
Book routine eye exams to monitor changes in your eyes, including the retina. Keeping a closer eye on your retina health can help preserve your vision and prevent retina conditions. We’re here to make your eye care as comfortable as possible. Request an appointment with Griffey Eye Care & Laser Center today.
Our Locations
Our Services
Our Testimonials
I recently went to my family doctor for pain I’d been having in my eye that was moving down my neck. I’d been waiting to have an MRI scheduled, and it was taking forever. I wanted to get a second opinion about what course of action should be taken. My husband and daughter are both patients at this practice and have always received stellar treatment. Dr. Griffey took very good care of me and went the extra step to send a letter to my family doctor while I was still there to concur with what they had said and also confirm that he would suggest an MRI as well. I was very impressed with him and his patient care. And, I appreciate the staff (particularly Tara and Benita) in scheduling me in as soon as possible. I would highly recommend this practice! Thank you all again for your help.
Beth K
I was referred to Dr. Griffey by several people. I was told he was an excellent ophthalmologist, and they were right. This was my first time meeting him and he made me feel so safe, comfortable and confident that he was providing me with the best and most knowledgeable treatment I could ask for. As I sat in the chair, I observed him interact with a baby he kissed on the forehead, it was so special to see him do that because it showed a gentle side of him, and his interaction with his assistants was nice, professional and straight to the point of what he needed in order to help his patient, I remember him saying to one of them that he was not going to let me leave until he reviewed a report from another doctor about my condition and that really made me feel special because it showed his concern. I don’t think I could have asked for a better doctor. Thank you Dr. Griffey for being the best and hats off to your father and grandfather.
C. Blount
I had a wonderful first appointment. The staff is attentive and the techs and doctors are knowledgeable and take their time really getting to know their patients. So happy to have found them.
M. Catherine
I travel from Atlanta, Georgia to see Dr. Griffey, MD, and board certified Ophthalmologist. Dr. Griffey has performed two surgeries on me and I would trust him to do anything he deems necessary. The staff is fantastic and I would recommend Dr. Griffey, to all that needed to see a competent Ophthalmologist!!!
M.Bailey Buck
I want to thank everyone at Chesapeake Eye Care for their care on a recent visit. I had an accident involving my eye and even though they were booked, the receptionist worked me in that day. The technician and Dr. Fox saw me promptly and performed a thorough exam. I was very pleased with both of them and appreciated their kindness and professionalism.
P. Brangan
My dad had cataract surgery a couple years ago. I was a little nervous for him, he’d been resisting getting surgery for so long. However, the staff and Dr. Griffey were wonderful to him and everything went very smoothly. He had a great experience, and I am thankful to them for making him so comfortable.
K. Kroll
The best thing I ever did was get LASIK surgery; it is unbelievable how I can see 20/20. When I get in bed at night I still think … wait….no, I don’t have to take my contacts out and it’s been 3 months. It was wonderful in Mexico also with not having to worry about contacts and all the solutions to bring with me. I had an amazing experience with my LASIK surgery with Dr. Paul Griffey and his staff! I would definitely recommend him to friends and family!!!
E. McConnell
I sent my mom to Dr. Griffey for a 2nd opinion on her eyes. Years later, I am still satisfied with the care he has provided. She had an appointment today and Dr. Griffey called me personally to discuss my concerns. WOW!!!!! GREAT PROVIDER!!!!!! I also referred my dad to him after a bad cataract surgery elsewhere. Dr Griffey did his 2nd eye without complications. THANK YOU for taking care of my parents! I have 30+ years in the business as a licensed optician and have worked with many doctors, I would recommend Dr. Griffey to any patient for care!!!!!!!!!!
Selena Cabral
I have been a patient of Dr. Griffey, since 2012. I’m born, raised, formal education, retired Law Enforcement, City of Virginia Beach, VA. After moving to Atlanta, I felt I could not find the care I needed, so I travel back and forth to receive my care. I will not allow anyone to see me. Well worth the trip, and will continue to do so!
Thank you for being The Best…
MBB
We both underwent cataract surgery, in both eyes. Barbara’s was in September of 2018. Mine was in December 2018. We both had excellent experiences, from her first visit, to my last. Dr. Griffey, as well as everyone on his staff, (that we came in contact with), were prompt and very professional. Yet, at the same time they were relaxed and very friendly. We were very impressed that everyone, asked, if we had any questions.
And, we can both see 20/20 again!!.
There was an general atmosphere of confidence and calmness throughout his practice, as well as within the Chesapeake Surgical Center. That made us both feel very comfortable, and well cared for. We have never before experienced such a well run practice. We have, (and will continue to), highly recommend Dr. Griffey to anyone who needs eye care.
Barbara and Eddie
CHECK US OUT ON SOCIAL


We are a proud partner of US Eye, a leading group of patient-centric, vertically integrated multi-specialty physician practices providing patients with care in ophthalmology, optometry, dermatology, audiology, and cosmetic facial surgery.